How is anesthesia used in canine surgery?
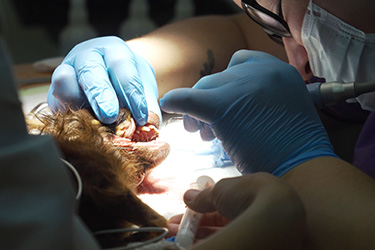
Just like humans, dogs are often put under anesthesia when receiving surgery. However, since conditions such as gingivitis and periodontal disease require anesthesia to treat, it’s no surprise that dog owners are concerned and desire to learn more about the process.
So, what happens when your dog has a general anesthetic, and are you right to be worried?
Pre-procedure tests
Before your dog has a dental procedure, the vet will carry out a number of tests to check for any existing health problems that could affect your dog’s suitability for general anesthesia. First, they should perform a general physical exam. Based upon the exam, other tests relevant to your dog’s age, medical history, and breed, may include a complete blood count (CBC), a thyroid test, a chemistry profile, and an ECG or Ultrasound if your dog’s heart has abnormal beats. The test results will enable the vet to choose the safest, most appropriate, and correct dose of drugs to use during your dog’s procedure.
You will be given the relevant consent paperwork to complete before the tests are undertaken, and this is your chance to ask any questions that you have about the procedure or to voice your concerns.
Preparing your dog for general anesthesia
Initially, your dog will be given a sedative to relieve anxiety and to alleviate any discomfort. An intravenous catheter is used to administer injectable anesthetics and fluids directly into the blood stream and is also available in case emergency medication is required during the procedure.
Dogs will often receive an intravenous anesthetic, followed by a gas anesthetic. Once your dog is anesthetized, an endotracheal tube will be placed in their trachea to protect their airway and to administer the gas that ensures they stay unconscious throughout the procedure.
Before, during, and after general anesthesia, intravenous fluids will be given to your dog to help keep their vital organs and kidneys hydrated and to assist with blood pressure maintenance.
Monitoring

Throughout your dog’s procedure, their vital signs will be closely monitored by a veterinary technician to ensure that they are doing well. Monitoring is essential to ensure your dog’s safety throughout the dental procedure.
Heart rhythm and rate
Your dog’s heart will be monitored to ensure that the rate and rhythm remain within normal parameters. An electrocardiogram (ECG, EKG) is often used for this purpose. An EKG measures the electrical impulses that the heart generates, allowing early recognition of any changes to the heart rhythm and rate.
Alternatively, an esophageal stethoscope may be used. This is a simple device that is placed down your dog’s esophagus to the level of their heart. The sound of the heart is then amplified through a speaker, allowing changes in rate or rhythm to be detected.
Blood flow and pressure
Efficient tissue perfusion is essential for your dog’s well-being during the procedure. Tissue perfusion refers to the movement of blood through the vessels in your dog’s organs. Perfusion is monitored through the measurement of capillary refill time (CRT). CRT is assessed by applying gentle pressure to your dog’s gums so that they turn pale and observing how long it takes for the gum color to return to normal. With good tissue perfusion, CRT should take about one second.
Most importantly, your dog’s blood pressure is also closely monitored to help determine the depth of anesthesia and tissue perfusion.
Oxygen saturation
Pulse oximetry will be carried out to ensure that your dog’s blood contains sufficient oxygen.
A sensory probe is clipped to any area of superficial vascularization such as the pink, unpigmented area of your dog’s tongue, a paw, the penis/vulva, etc. and the color of the mucous membranes is measured. Pink membranes normally indicate good oxygen saturation.
Respiratory rate
Your dog’s breathing and respiratory system function is monitored simply by observing the chest wall and counting the number of breaths that are taken per minute. In addition, the movement of the reservoir bag on the gas anesthetic machine is monitored.
Temperature
Your dog’s body temperature will fall slightly while under anesthetic. Your dog will be kept warm during the procedure through the use of heat pads and blankets, and his temperature will be monitored closely.
Depth of anesthesia
Throughout the procedure, the anesthetist will watch your dog closely for signs that might indicate that the anesthesia requires adjustment. These checks are made via visual observations, including pupil position, certain reflexes, and muscle relaxation.
General anesthesia for dogs
General anesthesia is used to keep your dog from moving while the procedure is carried out, to prevent pain, and to cause muscle relaxation. General gas anesthetics that are commonly used include halothane and isoflurane. Isoflurane is preferred when treating older dogs, as it places less strain on the heart and other organs, and is thus deemed to be safer.
There are two main types of gas anesthesia systems in use in small-animal practices: non-rebreathing and rebreathing, and both require close monitoring.
Rebreathing gas anesthesia systems
Rebreathing systems or partial rebreathing systems are generally used for larger dogs weighing more than 10 pounds or high risk cases. Each breath administered by the system contains exhaled gas where the carbon dioxide content has been removed and replaced by oxygen and anesthetic.
Rebreathing systems offer a number of advantages: Less anesthetic gases and oxygen are used because of lower flow rates, less waste gases are produced, and your dog’s moisture and heat from respirations are conserved.
Non-rebreathing gas anesthesia systems
Non-rebreathing gas anesthesia systems are typically used on small dogs that weigh less than 10 pounds. Smaller animals require a higher gas flow to prevent them from rebreathing carbon dioxide. This system sees very little or no exhaled gases retuned to your dog, being removed instead by the system.
The gas anesthesia machine mixes the anesthetic gas with oxygen and delivers it to your dog via the endotracheal tube. The gas then moves across the lungs until it reaches the alveoli. The gas is then transferred through the alveoli into the bloodstream and onward to the brain, where the state of anesthesia is achieved. To decrease the depth of anesthesia during the procedure or to awaken your dog, the process is reversed.
Canine recovery from general anesthesia
After the procedure, your dog will be placed somewhere warm and quiet, but under observation, while recovering from the anesthesia. Ideally, they should awaken slowly and quietly. Urination and vomiting is not uncommon as your dog comes round from the anesthetic, and shivering is quite normal as the body’s temperature regulation mechanism stabilizes. While they recover, your dog’s vital signs will be closely monitored.
Following routine dental procedures, most dogs are ready to go home after four to eight hours.
If your dog is having teeth removed or will be in discomfort when they awaken, your vet will give pain-relieving medication immediately following the procedure so that it is already working when your dog wakes up. Other medications will be given as required on a case by case basis.
If your dog is pawing at their mouth, an Elizabethan collar may be fitted.
Your dog may feel nauseous and sleepy for 24 hours following the procedure. Allow them to sleep off the anesthetic, and be sure that they have fresh water readily available.
Canine anesthesia facts
- General anesthesia is used for most canine dental procedures.
- Your dog’s vital signs will be closely monitored throughout his anesthesia.
Although no surgical procedure is 100% risk-free, anesthesia is generally very safe!
About Dr. James Anthony
Dr. James Anthony has been involved in veterinary medicine for
over 30 years. He is a boarded Veterinary Dentist since 1989 (Diplomate of the AVDC).
Dr. Anthony has had an extensive academic career as well, having
taught veterinary dentistry at the University of Guelph, the University of Montreal and the University of Prince Edward Island. He was also a Tenured Professor at the University of Saskatchewan as the Head of
Veterinary Oral Surgery and Dentistry.
Dr. Anthony has authored over 40 articles and book chapters, and throughout his career has lectured globally at veterinary meetings.
Original article: https://1tdc.com/how-is-anesthesia-used-in-canine-surgery/


Working Here
Our team members are encouraged to be the best they can be... at Covetrus we believe we impact one another.
Learn MoreNews & Events
FDA Cautions Pet Owners Not to Feed Texas Tripe Inc. Raw Pet Food Due to Salmonella, Listeria Monocytogenes
The U.S. Food and Drug Administration is cautioning pet owners not to feed their pets any of the Texas Tripe brand raw frozen pet food listed below because several samples of Texas Tripe raw pet food have tested positive for Salmonella and/or L. mono.
Careers
Are you looking for a place to let your talents shine? At Covetrus, we help our practitioner customers better serve their patients and take pride in providing the best customer experience possible. Search our open positions to see our available opportunities.
Newsletter
Stay current with what’s going on with Covetrus, subscribe to receive our newsletter and email communications. Subscribers will receive the latest information in practice management, sales and marketing, animal health, and more.



-3-(1).png?sfvrsn=2d806d73_0)

Leave a comment